What is plantar fasciitis?
Plantar fasciitis is the most common cause of heel pain, and most commonly occurs between ages 40 to 60 years. In chronic cases, viewing the plantar fascia under a microscope (histological analysis) shows no signs of inflammatory cells invading the fascia. Instead the tissue shows fibrosis and degenerative changes.
How is plantar fasciitis diagnosed?
Plantar fascia is a clinical diagnosis, but ultrasound and x-rays can be used to support the diagnosis.
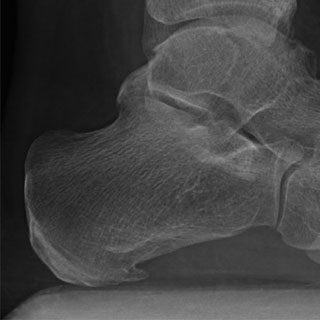
X-ray showing small calcaneal spur.
How is plantar fasciitis treated?
The mainstay of plantar fasciitis treatment is conservative management, including stretching, nonsteroidal anti-inflammatory drugs (NSAIDs), physical therapy and night splints. These traditional treatments are helpful in the majority of cases, provide with 80-90% of patients responding to conservative treatment (Shetty et al, 2019; Monteagudo et al 2013).
Do you perform steroid injections?
We typically discourage patients from getting steroid injections. While steroids (cortisone) injection can be effective for short-term relief, their role in treatment plantar fasciitis is questionable. Steroids are an anti-inflammatory and studies have shown that plantar fasciitis is not an inflammatory process. In addition, steroids can have potentially disabling complications such as plantar fascia rupture and fat pad atrophy (Shetty et al, 2019).
Do you recommend surgery for plantar fasciitis?
Surgery is indicated when plantar fascia does not respond to all nonoperative interventions, with reported success rates of 67 to 82% (Saxena et al, 2013; Lundeen et al, 2000). Complete surgical release can alter foot biomechanics with loos of the windlass effect after surgery. Endoscopic partial fasciotomy avoids these complications, but a recent review only identified 12 articles assessing the efficacy of endoscopic fasciotomy with the majority of the level of evidence was low (level IV). While there seemed to be good outcomes for endoscopic plantar fasciotomy, the systematic review could only offer a grade C recommendation for the procedure (Mao et al, 2019).
What if I do not want surgery? What if I did not improve after surgery?
Platelet rich plasma (PRP) and ultrasonic fasciopathy with Tenex are both minimally invasive treatment options for chronic plantar fasciitis. Tenex has been shown to be helpful in cases of plantar fasciitis that have not previously responded to surgery (Razdan et al, 2015).
Does PRP work for Plantar Fasciitis?
PRP demonstrated better results in the long-term than steroid injections for pain control and functional outcomes
How does plantar rich plasma (PRP) work for plantar fasciitis?
Plantar rich plasma, or PRP, has been used in orthopedics since the early 2000s and has been well studied in plantar fasciitis. Second to tennis elbow, plantar fasciitis is the best studied orthopedic indication. In the past year 4 high level randomized controlled studies have compared PRP to steroid injections or phonophoresis showing good long-term results and decreased need for surgery in the majority of studies (Peerbooms et al, 2019; Gonnade et al, 2018; Malahias et al, 2019; Shetty et al 2019).
PRP concentrates a patient’s blood to increase various growth factors. When injected into the injured plantar fascia it stimulates the natural healing response. Since chronic plantar fasciitis is a chronic process stimulating a healing response addresses the underlying cause of pain.
How does Tenex work for plantar fasciitis?
Tenex uses ultrasonic technology to remove thickened diseased plantar fascia tissue and stimulate a healing response. The procedure is minimally invasive, and performed with ultrasound guidance. This minimizes any injury to surrounding tissue and allows for a targeted treatment only removing the diseased and pathologic abnormal fascia.
The procedure is performed using only local numbing around the plantar fascia and a nerve block so patient avoids any potential risk associated with general anesthesia. Unlike traditional surgery, patients typically only have to wear a walking boot for 5 days after the treatment and start stretching exercises immediately after the procedure. In addition, the procedure is typically covered by insurance.
For more information on minimally invasive PRP or Tenex treatments for plantar fasciitis schedule a consult at 781-591-7855.
References:
Gonnade N, Bajpayee A, Elhence A, et al. Regenerative efficacy of therapeutic quality platelet-rich plasma injections versus phonophoresis with kinesiotaping for the treatment of chronic plantar fasciitis: A prospective randomized pilot study. Asian J Transfus Sci. 2018.
Lundeen R, Aziz S, Burks J, et al. Endoscopic plantar fasciotomy: A retrospective analysis of results in 53 patients. J Foot Ankle Surg. 2000.
Malahias MA, Mavrogenis AF, Nikolaou VS, et al. Similar effect of ultrasound-guided platelet-rich plasma versus platelet-poor plasma injections for chronic plantar fasciitis. Foot (Edinb). 2019.
Mao DW, Chandrakumara D, Zheng Q, et al. Endoscopic plantar fasciotomy for plantar fasciitis: A systematic review and network meta-analysis of the English literature. Foot (Edinb). 2019.
Monteagudo M, Maceira E, Garcia-Virto V, Canosa R. Chronic plantar fasciitis: plantar fasciotomy versus gastrocnemius recession. Int Orthop. 2013.
Patel M. A novel treatment method for refractory plantar fasciitis. American Journal of Orthopedics. 2015.
Peerbooms JC, Lodder P, den Oudsten BL, et al. Positive Effect of Platelet-Rich Plasma on Pain in Plantar Fasciitis: A Double-Blind Multicenter Randomized Controlled Trial. Am J Sports Med. 2019.
Razdan R, Vanderwoude E, Braun A, Morrey B. Percutaneous Ultrasonic Fasciotomy: A Novel Approach to Treat Chronic Plantar Fasciitis. J Surg Proced Tech. 2018.
Saxena A, Fournier M, Gerdesmeyer L, et al. Comparison between extracorporeal shockwave therapy, placebo ESWT and endoscopic plantar fasciotomy for the treatment of chronic plantar heel pain in the athlete. Muscles Ligaments Tendons J. 2013.
Shetty SH, Dhond A, Arora M, Deore S. Platelet-Rich Plasma Has Better Long-Term Results Than Corticosteroids or Placebo for Chronic Plantar Fasciitis: Randomized Control Trial. J Foot Ankle Surg. 2019.
Ultrasound-guided tendon scraping is an emerging minimally invasive treatment for patellar tendinitis (jumper’s knee). A recent study shows promising results with faster return to sport and significant pain relief,
Read MorePatellar tendinitis (“jumper’s knee”) is a common cause of knee pain in athletes. Learn what causes it, why it lingers, and how advanced treatments like ultrasound-guided tendon scraping may help you recover faster and
Read More