Dr. Sussman is one of the first doctors in the Greater Boston region to be trained on Tenex and has performed more Tenex procedures than anyone in New England. Tenex is a groundbreaking technology and offers a safe, quick, minimally invasive solution to tendon pain. The procedure is performed in less than 20 minutes, patients are awake and alert throughout (only a local anesthetic is used), and no sutures or stitches are needed. Patients leave with only a small adhesive bandage and return to activity than with open tendon surgeries with most patients are able to return to normal activity within 2-6 weeks.
One of the most common tendons treated with Tenex is the outside of the elbow for lateral epicondylitis or tennis elbow. Lateral epicondylitis is common affecting 1-3% of the general population and up to 29.3% of people doing heavy labor.[2] In some patients, symptoms can linger for 6 to 24-months,[3, 4] and patients with more than 6-months of pain are less likely to experience spontaneous resolution of their symptoms.[5, 6]
In the past month, a study from the Cleveland Clinic and University of Pennsylvania compared Tenex to surgery for lateral epicondylitis. In the study, the authors found that Tenex had similar outcomes to open surgical tenotomy at 3, 6 and 12-months after the procedure.[1]

Tenex is an innovative treatment for chronic tendon pain. Tenex uses ultrasonic energy to debride and remove abnormal tissue. The Tenex system (Image A) uses a needle, which vibrates at a low-frequency and removes diseased degenerative tendon tissue. The double lumen needle design (Image B) allows the Tenex needle to irrigate the disease tendon with pressurized fluid, and has a vacuum mechanism to then remove the fluid and disease tissue.

How does Tenex compare to surgery?
Surgery uses an incision to visualize the tendon and sometimes the surgeon has to cut healthy tendon to get to the abnormal pathologic tissue. Tenex uses ultrasound to guide the microtip into the diseased areas of the tendon, which preserves health tendon and allows us to only target and remove the unhealthy tendon tissue. This allows patients to return to activity faster after Tenex than with open surgery with no difference in long-term outcomes.
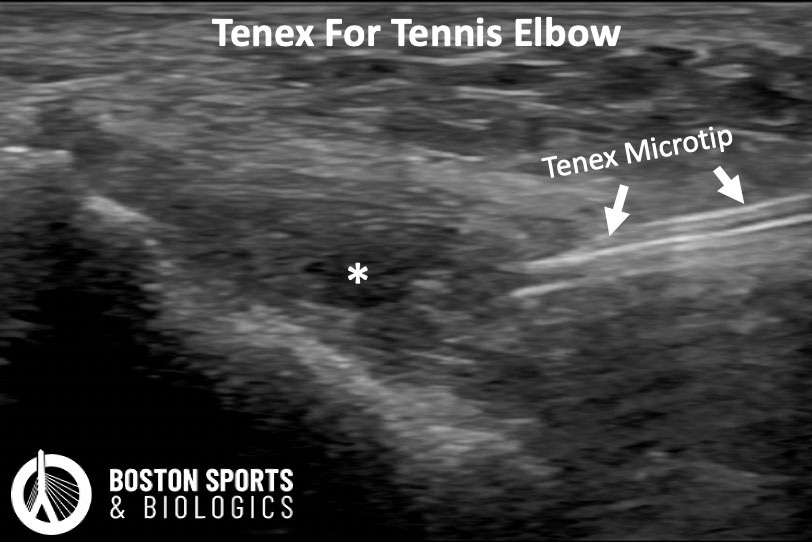
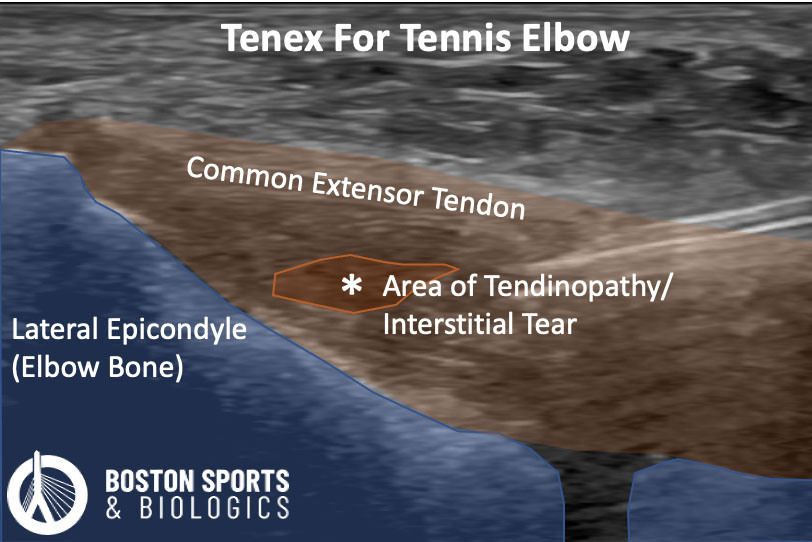
What can you treat with Tenex?
Studies have examined the use of Tenex percutaneous needle tenotomy in lateral and medial epicondylitis, triceps tendinopathy, gluteal tendinopathy, patellar tendinopathy, Achilles tendinopathy, plantar fasciitis, and peroneal tendinopathy.
A new Tenex Bone needle allows us to remove bone spurs or extra-bone.
REFERENCES
1. Altahawi F, Li X, Demarest B, Forney MC. Percutaneous ultrasonic tenotomy with the TX-1 device versus surgical tenotomy for the treatment of common extensor tendinosis. Skeletal Radiol. 2020.
2. Shiri R, Viikari-Juntura E. Lateral and medial epicondylitis: role of occupational factors. Best Pract Res Clin Rheumatol. 2011; 25(1):43-57.
3. Faro F, Wolf JM. Lateral epicondylitis: review and current concepts. J Hand Surg Am. 2007; 32(8):1271-1279.
4. Coonrad RW, Hooper WR. Tennis elbow: its course, natural history, conservative and surgical management. J Bone Joint Surg Am. 1973; 55(6):1177-1182.
5. Sanders TL, Maradit Kremers H, Bryan AJ, Ransom JE, Morrey BF. Health Care Utilization and Direct Medical Costs of Tennis Elbow: A Population-Based Study. Sports health. 2016; 8(4):355-358.
6. Sanders TL, Jr., Maradit Kremers H, Bryan AJ, Ransom JE, Smith J, Morrey BF. The epidemiology and health care burden of tennis elbow: a population-based study. Am J Sports Med. 2015; 43(5):1066-1071.
7. Boden AL, Scott MT, Dalwadi PP, Mautner K, Mason RA, Gottschalk MB. Platelet-rich plasma versus Tenex in the treatment of medial and lateral epicondylitis. Journal of shoulder and elbow surgery / American Shoulder and Elbow Surgeons [et al]. 2019; 28(1):112-119.
Ultrasound-guided tendon scraping is an emerging minimally invasive treatment for patellar tendinitis (jumper’s knee). A recent study shows promising results with faster return to sport and significant pain relief,
Read MorePatellar tendinitis (“jumper’s knee”) is a common cause of knee pain in athletes. Learn what causes it, why it lingers, and how advanced treatments like ultrasound-guided tendon scraping may help you recover faster and
Read More