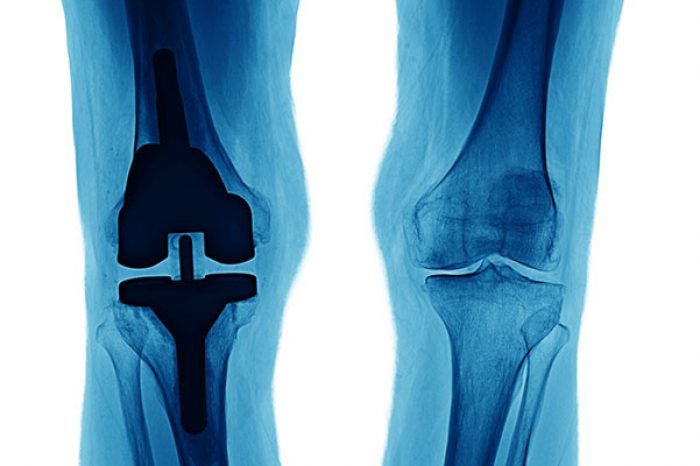
There has been a sharp rise in knee osteoarthritis in younger patients. During the 1990s, the average age of patients diagnosed with knee osteoarthritis was 72-years-old. In 2016, over half of patients were less than 65-years-old (Deshpande et al 2016). With the sharp rise in knee osteoarthritis in younger patients a different approach and new management strategies are needed.
“How long does a knee replacement lasts” is a frequently question we get in clinic. Unfortunately, it’s difficult to predict how long a joint replacement will last.
The goal of a total knee replacement surgery is to provide long-term relief from knee pain, but knee replacements can fail for a variety of reasons. Given enough time all knee replacements will fail and need revision surgery. Younger patients tend to be more active and put more stress on joint replacements. For these reasons, some surgeons advise younger patients to put off surgery for as long as possible.
In one large study with over 63,000 patients, age did influence the need for revision surgery. In patients over 70-years-old, the lifetime risk of having a second operation was about 5%. This risk was much greater in younger individuals. In this study, 35% of men in their early 50s required a second operation (Bayliss et al 2017).
Patient's satisfaction with a knee replacement varies across studies, but in general one in five patients are dissatisfied after total knee replacement (Beswick et al 2012; Bert et al 2018). In general, the longevity of a total knee replacements is greater than 10 years. In one review and meta-analysis one patient in every 25 (3.9%) required a revision surgery within 10-years of a total knee replacement. Approximately one patient in every 10 (10.3%) required a revision surgery within 20-years of the knee replacement (Bayliss et al 2017), but not all patients with complications opted for a revision surgery.
Age influences the need for revision surgery
The need for revision surgeries is projected to grow with younger age of diagnosis and dissatisfaction rates, and points to the need for alternative therapy and management.
When a hip or knee joint is “worn out” and conservative treatments such as medications or steroid injections aren’t helping there aren’t many good options. At this stage patients are typically offered a total knee replacement.
Not all patients with advanced knee osteoarthritis are candidates for a total knee replacement. Other patients may prefer to delay or avoid surgery altogether.
In these cases, we typically offer patients platelet rich plasma (PRP), stem cell (BMAC), or hyaluronic acid (HA)/viscosupplementation injections to postpone a total knee arthroplasty
Viscosupplementation or HA injections have been used worldwide for decades, and have been approved for the use in the United States since 1997. Research has demonstrated that HA injections result in decreased pain and improved function, and can help delay a total knee replacement (Gannuru et al 2009; Day et al 2004; Tang et al 2008).
HA works through various mechanisms. In osteoarthritis, the concentration and molecular weight of the natural hyaluronic acid within the joint fluid changes. This diminishes the viscoelastic and protective properties of the joint fluid (Ghosh and Guidolin 2002).
Hyaluronic acid injections help the lubrication and improve the viscoelasticity to the synovial joint fluid. Different HA formulations exist, and each preparation has a different molecular weight, ranging from 2 to 10 million Daltons (Da). Supplementing the joint with HA injections can help with pain relief, improved function, and reduced stiffness.
In addition, HA injections have been shown to reduce inflammatory cytokines such as interleukin-1 (Larsson et al 2004; Waddell et al 2007). Furthermore, HA may offer protective properties to the joint tissue by scavenging free radicals and reducing oxidative damage (Ghosh and Guidolin 2002).
Several studies have found hyaluronic acid injections are successful in delaying a total knee replacement. How long patients feel better after a HA injection varies, but on average most patients can achieve benefit for up to 2 years and sometimes longer (Ayhan et al 2014).
One study using a database of 182,022 patients who had a total knee replacement found that repeated hyaluronic acid injections were able to delay the need for the surgery for over 3-years (Altman et al. 2015). In this study, those who did not get the injections had the surgery within 0.7 years, those with one course of injections had the surgery in 1.4 years, and patient who repeated the injection five times delayed surgery by 3.6 years. Similar results have been shown in other studies (Delbarre et al, 2017)
Can viscosupplementation or Hyaluronic Acid (HA) injections help delay a total knee replacement surgery?
In one study, repeated hyaluronic acid injections were shown to delay total knee replacement surgery for over 3-years in patients with knee osteoarthritis
Viscosupplementation injection can be a good option for patients who are note candidates for surgery or are looking to delay a total knee replacement. Osteoarthritis of the knee is the most common type of arthritis in the United States, affecting an estimated 13.7 million people. Intra-articular HA injection has been in clinical use worldwide for decades to help patients find relief.
Studies have attempted to identify which patients are good candidates for HA injections. Certain subgroups of patients may respond to HA and other may not benefit from these injections. Most studies have examined patients with mild to moderate osteoarthritis, but some studies evaluating patients with severe osteoarthritis found HA useful (Blanco et al, 2008). There is no consensus or existing clinical guidelines that offer recommendations for subsets of patient care.
HA injections are considered safe and an effective means of treating pain and disability patients with knee osteoarthritis. The most common adverse reaction to HA injections is transient injection site pain which typically resolves.
Patients with skin disease or infection around the knee should delay the procedure until the skin infection or disease is managed and it is safe to give the injection. Inflammatory arthritis is also a contraindication for HA injections.
In Massachusetts, most insurances cover HA injections. MassHealth and Blue Cross and Blue Shield do not typically cover viscosupplementation injections, and these have to be covered by the patient as an out-of-pocket expense.
One of the reasons is that in 2013, the American Academy of Orthopaedic Surgeons (AAOS) released new clinical practice guideline (CPG) for the treatment of knee OA and changed their recommendation from HA injections being “inconclusive” to “cannot recommend” based on the current studies. The analysis and recommendation does not reflect the real-world impact of HA injections. While HA injections may not reverse the arthritis, it has been shown to delay the need for a total knee replacement and can be particularly helpful for patients looking to put off surgery.
The criteria used by the AAOS may have been based on flawed methodology and interpretation of minimal clinically important differences. There have been growing calls to reconsider and modify these recommendations due to the impact on patient care when Blue Cross and Blue Shield and other plans decided not to pay for HA injections (Vangsness et al 2020).
All of the viscosupplementation injections are performed using ultrasound guidance, and ultrasound guided injections are more accurate than landmark guided injections. The location of the injection may also improve outcomes. In one study, patients that were injected along the midpatella had greater pain relief and satisfaction compared to the anterior or the front of the knee (Xiao et al. 2021).

Altman R, Lim S, Steen RG, Dasa V. Hyaluronic acid injections are associated with delay of total knee replacement surgery in patients with knee osteoarthritis: Evidence from a large U.S. Health claims database [published correction appears in PLoS One. 2016;11(1):e0148591]. PLoS One. 2015;10(12):e0145776.
American Academy of Orthopaedic Surgeons. Viscosupplementation for knee arthritis. Updated June, 2015.
Ayhan E, Kesmezacar H, Akgun I. Intraarticular injections (corticosteroid, hyaluronic acid, platelet rich plasma) for the knee osteoarthritis. World J Orthop. 2014 Jul 18; 5(3):351-61.
Bayliss LE, Culliford D, Monk AP, Glyn-Jones S, Prieto-Alhambra D, Judge A, Cooper C, Carr AJ, Arden NK, Beard DJ, Price AJ. The effect of patient age at intervention on risk of implant revision after total replacement of the hip or knee: a population-based cohort study. Lancet. 2017 Apr 8;389(10077):1424-1430.
Bert J, Kenney J, Sgaglione NA, McClelland S, Brophy R, Toth J, Ruane J, Ali Y, Arquette S, Dasa V, Lopes M. Viscosupplementation for Osteoarthritis of the Knee: A Key Opinion Leader Panel Discussion. J Manag Care Spec Pharm. 2018 Jun;24(6-a Suppl):S2-S8.
Beswick AD, Wylde V, Gooberman-Hill R, Blom A, Dieppe P. What proportion of patients report long-term pain after total hip or knee replacement for osteoarthritis? A systematic review of prospective studies in unselected patients. BMJ Open. 2012; 2: e000435
Blanco, F, Fernandez-Sueiro, J, Pinto-Tasende, J, Fernandez-Lopez, J, Ramallal, M, Freire, A. Intra-articular hyaluronan treatment of patients with knee osteoarthritis waiting for replacement surgery. Open Arthritis J. 2008;1:1-7.
Delbarre A, Amor B, Bardoulat I, Tetafort A, Pelletier-Fleury N. Do intra-articular hyaluronic acid injections delay total knee replacement in patients with osteoarthritis - A Cox model analysis. PLoS One. 2017; 12(11):e0187227.
Deshpande BR, Katz JN, Solomon DH, et al. Number of persons with symptomatic knee osteoarthritis in the U.S.: impact of race and ethnicity, age, sex, and obesity. Arthritis Care Res (Hoboken). 2016;68(12):1743-50.
Ghosh P, Guidolin D. Potential mechanism of action of intra-articular hyaluronan therapy in osteoarthritis: are the effects molecular weight dependent? Semin Arthritis Rheum. 2002 Aug; 32(1):10-37
Larsson E, Erlandsson Harris H, Larsson A, Mansson B, Saxne T, Klareskog L. Corticosteroid treatment of experimental arthritis retards cartilage destruction as determined by histology and serum COMP. Rheumatology (Oxford). 2004;43(4):428-34.
Vangsness, C. Thomas Jr. MD1,a; Adamson, Thomas C. III MD, FACP, CPE2; Daley, Michael J. PhD3 Consequences on Private Insurance Coverage, The Journal of Bone and Joint Surgery: May 20, 2020 - Volume 102 - Issue 10 - p 920-926
Waddell DD, Kolomytkin OV, Dunn S, Marino AA. Hyaluronan suppresses IL-1beta-induced metalloproteinase activity from synovial tissue. Clin Orthop Relat Res. 2007;465:241-8.
Xiao J, Hu Y, Huang L, Huang ZF, Jiang WZ, Luo YQ, Jia MY, Chen D, Shi ZJ. Injection route affects intra-articular hyaluronic acid distribution and clinical outcome in viscosupplementation treatment for knee osteoarthritis: a combined cadaver study and randomized clinical trial. Drug Deliv Transl Res. 2021 Feb;11(1):279-291.
Ultrasound-guided tendon scraping is an emerging minimally invasive treatment for patellar tendinitis (jumper’s knee). A recent study shows promising results with faster return to sport and significant pain relief,
Read MorePatellar tendinitis (“jumper’s knee”) is a common cause of knee pain in athletes. Learn what causes it, why it lingers, and how advanced treatments like ultrasound-guided tendon scraping may help you recover faster and
Read More