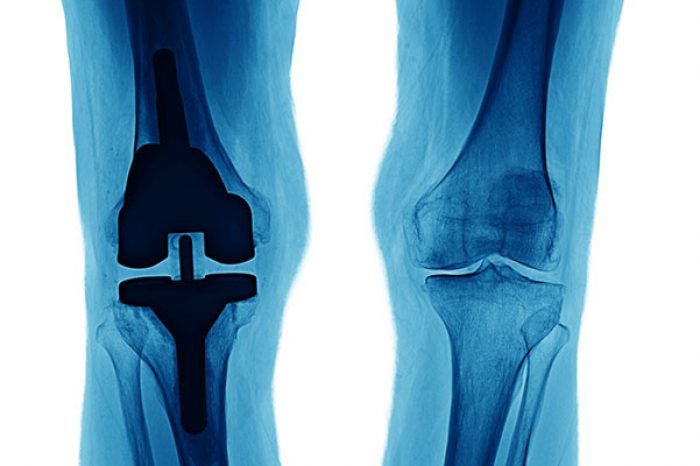
Knee arthritis is one of the most common causes of pain, stiffness, and loss of mobility in active adults. If you’ve been told you have “bone-on-bone” arthritis, a bone marrow lesion, or that knee replacement is your next step, you may be searching for alternatives.
Many patients in Greater Boston are now asking about stem cell injections for knee osteoarthritis.
This guide explains what these treatments are, how they work, who may benefit, and what to realistically expect.
Knee osteoarthritis (OA) has traditionally been described as “wear and tear” of cartilage. But modern research shows something important, the subchondral bone (the bone just beneath the cartilage) plays a major role in pain and progression.
When the bone becomes inflamed, overloaded, or develops bone marrow lesions (BMLs), patients often experience deep, aching pain — especially with weight bearing.
The subchondral bone sits directly beneath the cartilage surface.
In knee arthritis:
The bone can become hardened (sclerosis)
Small cracks or stress reactions can form
Bone marrow lesions may develop
Pain signals increase
This is one reason why some traditional joint injections don’t fully relieve symptoms — they treat the joint space but not the bone beneath it.
On MRI, a bone marrow lesion appears as a bright signal within the bone under the cartilage.
Patients often hear:
“Bone bruise”
“Subchondral edema”
“Bone stress reaction”
Research shows:
BMLs correlate strongly with knee pain
They are associated with faster cartilage breakdown
Larger BMLs increase risk of progression to knee replacement
This is where intraosseous BMAC injections may play a role.
A BMAC knee injection uses your own bone marrow, typically harvested from the back of the pelvis.
The marrow is processed into bone marrow aspirate concentrate (BMAC), which contains:
Mesenchymal stem cells (MSCs)
Hematopoietic cells
Growth factors
Anti-inflammatory cytokines
Platelets
While often referred to as “stem cell injections,” BMAC is technically a cellular concentrate containing regenerative and signaling cells (Schäfer et al, 2019; El-Jawhari et al, 2020). The characterization of BMAC as distinct from embryonic stem cells and donor tissue is accurate. BMAC is classified as an autologous, minimally manipulated cellular therapy. BMAC often qualifies under the Same Surgical Procedure Exemption or is regulated through its processing devices rather than as an FDA-approved therapeutic itself. This regulatory distinction reflects that BMAC uses the patient's own biologic material with minimal manipulation.
Intra-Articular Injection
Injected directly into the joint space. Common for:
Cortisone
Hyaluronic acid
PRP
BMAC
These target:
Synovial inflammation
Cartilage surface
Joint lining
Intraosseous Injection
Injected directly into the subchondral bone under imaging guidance.
These target:
Bone marrow lesions
Subchondral inflammation
Bone remodeling
Emerging evidence suggests that addressing both the joint and the bone may provide more durable symptom improvement in selected patients.
Research in orthobiologics continues to evolve. Studies have demonstrated:
Improved pain scores after BMAC injections
Functional improvement in selected patients
BMAC demonstrates significant functional improvements across multiple validated outcome measures. A 4-year prospective study of severe OA (KL grade III-IV) showed IKDC scores increased from 56 ± 12 to 73 ± 13 (P < 0.001) and WOMAC decreased from 40 ± 23 to 18 ± 18 (P < 0.001), with 95% of knees showing improvement and no prostheses required. (Pabinger et al, 2024)
A Level I meta-analysis found BMAC produced significantly better WOMAC (P < .001), VAS (P = .03), and IKDC scores (P < .001) compared to hyaluronic acid, with no significant differences compared to PRP (Belk et al, 2023).
Potential benefit in patients with bone marrow lesions
A prospective multicenter pilot study specifically targeting patients with subchondral bone alterations found that combined intra-articular and subchondral BMAC injections produced significant bone marrow edema reduction on MRI (P = 0.003), along with significant improvements in IKDC (40.5 to 62.6), VAS pain, and all KOOS subscales at 12 months. (Kon et al, 2021)
Longer symptom duration compared to corticosteroids
A network meta-analysis with minimum 6-month follow-up found that PRP, BMAC, and HA all outperformed corticosteroids in pain and function scores. Corticosteroids reach maximum pain control at 4-6 weeks but show equivalent outcomes to placebo by 6 months, whereas biologic therapies maintain benefits longer. (Jawanda et al, 2024)
While large randomized trials are ongoing, early clinical data and mechanistic understanding of subchondral bone pathology support further investigation.
BMAC uses your own minimally manipulated bone marrow. It is regulated under same-day autologous use guidelines. It is not FDA approved as a “drug,” but is commonly used in orthopedic procedures.
Results vary. Some patients report improvement lasting 1–3 years. Others may require repeat treatment or ultimately choose surgery.
They are different biologic products. PRP focuses on platelet-derived growth factors. BMAC contains a broader cellular population. Selection depends on severity and MRI findings.
There is no guarantee. However, some patients experience meaningful symptom relief that allows them to delay surgery.
The harvest is performed under local anesthesia. Most patients tolerate it well and describe soreness for a few days.
Belk JW, Lim JJ, Keeter C, McCulloch PC, Houck DA, McCarty EC, Frank RM, Kraeutler MJ. Patients With Knee Osteoarthritis Who Receive Platelet-Rich Plasma or BoneMarrow Aspirate Concentrate Injections Have Better Outcomes Than Patients Who Receive Hyaluronic Acid: Systematic Review and Meta-analysis. Arthroscopy. 2023 Jul;39(7):1714-1734. doi: 10.1016/j.arthro.2023.03.001. Epub2023 Mar 11. PMID: 36913992.
El-Jawhari JJ, Ilas DC, Jones W, Cuthbert R, Jones E, Giannoudis PV. Enrichment and preservedfunctionality of multipotential stromal cells in bone marrow concentrateprocessed by vertical centrifugation. Eur Cell Mater. 2020 Aug 4;40:58-73.doi: 10.22203/eCM.v040a04. PMID: 32749666.
Jawanda H, Khan ZA, Warrier AA, Acuña AJ, Allahabadi S, Kaplan DJ, Ritz E, Jackson GR, Mameri ES, Batra A, Dornan G, Westrick J, Verma NN, Chahla J. Platelet-Rich Plasma, Bone Marrow Aspirate Concentrate, and Hyaluronic Acid Injections Outperform Corticosteroids in Pain and Function Scores at a Minimum of 6 Months as Intra-Articular Injections for Knee Osteoarthritis: A Systematic Review and Network Meta-analysis. Arthroscopy. 2024 May;40(5):1623-1636.e1. doi: 10.1016/j.arthro.2024.01.037. Epub 2024 Feb 7. PMID: 38331363.
Keeling LE, Belk JW, Kraeutler MJ, Kallner AC, Lindsay A, McCarty EC, Postma WF. Bone Marrow Aspirate Concentrate for the Treatment of Knee Osteoarthritis: A Systematic Review. Am J Sports Med. 2022 Jul;50(8):2315-2323. doi: 10.1177/03635465211018837. Epub 2021 Jul 8. PMID: 34236913.
Kon E, Boffa A, Andriolo L, Di Martino A, Di Matteo B, Magarelli N, Marcacci M, Onorato F, Trenti N, Zaffagnini S, Filardo G. Subchondral and intra-articular injections of bone marrow concentrate are a safe and effective treatment for knee osteoarthritis: a prospective, multi-center pilot study. Knee Surg Sports Traumatol Arthrosc. 2021 Dec;29(12):4232-4240. doi: 10.1007s00167-021-06530-x. Epub 2021 Mar 27. PMID: 33772602.
Pabinger C, Lothaller H, Kobinia GS. Intra-articular injection of bone marrow aspirate concentrate (mesenchymal stem cells) in KL grade III and IV knee osteoarthritis: 4 year results of 37 knees. Sci Rep. 2024 Feb 1;14(1):2665. doi: 10.1038/s41598-024-51410-2. PMID: 38302491; PMCID:PMC10834500.
Schäfer R, DeBaun MR, Fleck E, Centeno CJ, Kraft D, Leibacher J, Bieback K, Seifried E, Dragoo JL. Quantitation of progenitor cell populations and growth factors after bone marrow aspirate concentration. J Transl Med. 2019 Apr 8;17(1):115. doi: 10.1186/s12967-019-1866-7. PMID: 30961655; PMCID: PMC6454687.
Ultrasound-guided tendon scraping is an emerging minimally invasive treatment for patellar tendinitis (jumper’s knee). A recent study shows promising results with faster return to sport and significant pain relief,
Read MorePatellar tendinitis (“jumper’s knee”) is a common cause of knee pain in athletes. Learn what causes it, why it lingers, and how advanced treatments like ultrasound-guided tendon scraping may help you recover faster and
Read More