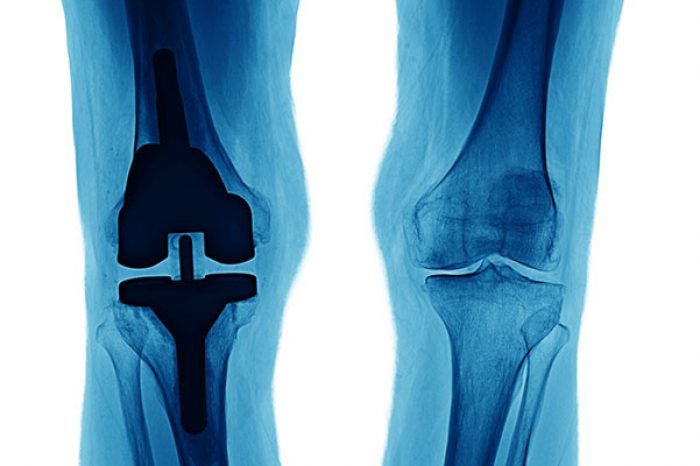
If you’ve had an MRI for knee arthritis, you may have seen the term “bone marrow edema” or “bone marrow lesion” (BML) in your report. Patients often ask:
The short answer is that bone marrow lesions are important. They are not just incidental findings. They are strongly associated with pain and with progression of knee osteoarthritis. Understanding them helps us better understand your knee pain, and may open the door to more targeted treatments.
On MRI, a bone marrow lesion appears as an ill-defined bright area in the bone just beneath the cartilage (the subchondral bone). Historically, this was called “bone marrow edema,” implying simple swelling. But research shows it’s more complex than that. Learn more about knee osteoarthritis here.
A landmark MRI–histology study by Zanetti et al. in Radiology found that what we call “bone marrow edema” on MRI is often not primarily fluid. Instead, it commonly contains:
Bone marrow necrosis
Fibrosis
Abnormal trabecular bone
Increased remodeling
In other words, a BML represents stressed, injured, and actively remodeling bone, not just inflammation.
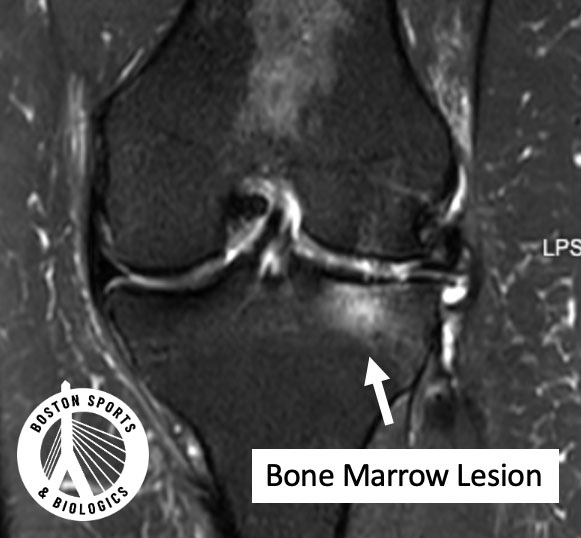
Cartilage itself does not have pain fibers. Bone does.
Subchondral bone is richly innervated. When it becomes overloaded, microfractured, or inflamed, it can generate significant pain signals.
A study in Osteoarthritis and Cartilage showed that:
Larger bone marrow lesions (>1 cm) were more common in patients with painful OA
The combination of full-thickness cartilage loss plus adjacent subchondral abnormalities was strongly associated with pain
This helps explain why some patients with mild X-ray arthritis have significant pain — and why others with severe X-ray arthritis have surprisingly little discomfort. The bone response may be the key driver.
Yes — and this is where things get clinically important.
A pivotal longitudinal study in Annals of Internal Medicine followed patients with symptomatic knee OA and found:
Knees with bone marrow lesions were 6-fold more likely to show medial progression
Lateral lesions conferred increased risk of lateral progression
Malalignment amplified the risk
In short:
Bone marrow lesions are not just markers of current pain — they predict structural deterioration.
Another study demonstrated that patients with BMLs were nearly 9 times more likely to progress to total knee replacement within 3 years, especially those with a “global” edema pattern (Scher et al, 2008).
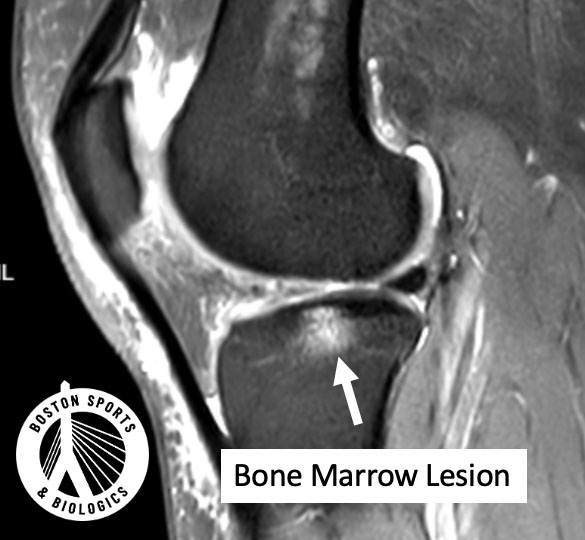
You may also see “subchondral cyst” on your MRI or CT report.
Cysts are fluid-filled cavities within the bone, often developing adjacent to areas of bone marrow lesions. A 2019 QCT study demonstrated that:
Greater cyst number and volume were associated with altered subchondral bone density
Cyst burden correlated with OA severity and joint space narrowing
Cysts reflect ongoing bone remodeling and stress. They are another sign that the subchondral bone is biologically active — not inert.
You should discuss it seriously with your physician if:
Remember:
Not every BML means surgery is imminent.
But ignoring it may allow continued structural stress.
In recent years, there has been increasing interest in targeting the subchondral bone directly.
The rationale:
BMLs represent areas of microfracture and abnormal remodeling.
Increased intraosseous pressure may contribute to pain.
Altering the biologic environment of the subchondral bone may reduce pain and potentially slow progression.
Research has shown that reducing intraosseous pressure in other conditions can relieve pain (Sowers et al. 2003).
This has led to the development of intra-osseous injection techniques, where biologic agents (such as PRP or bone marrow concentrate) are delivered directly into areas of subchondral bone abnormality under image guidance.
The goal is to:
Improve bone remodeling
Reduce microfracture stress response
Modulate inflammation
Potentially stabilize the osteochondral unit
While more high-quality studies are needed, this represents a shift from “surface-level” cartilage treatment to deep structural intervention.
Learn more about intra-osseous injections here.
Burnett WD, Kontulainen SA, McLennan CE, Hazel D, Talmo C, Wilson DR, Hunter DJ, Johnston JD. Knee osteoarthritis patients with more subchondral cysts have altered tibial subchondral bone mineral density. BMC Musculoskelet Disord. 2019 Jan 5;20(1):14. doi: 10.1186/s12891-018-2388-9. PMID: 30611224; PMCID: PMC6320646.
Felson DT, Chaisson CE, Hill CL, Totterman SM, Gale ME, Skinner KM, Kazis L, Gale DR. The association of bone marrow lesions with pain in knee osteoarthritis. Ann Intern Med. 2001 Apr 3;134(7):541-9. doi: 10.7326/0003-4819-134-7-200104030-00007. PMID: 11281736.
Scher C, Craig J, Nelson F. Bone marrow edema in the knee in osteoarthrosis and association with total knee arthroplasty within a three-year follow-up. Skeletal Radiol. 2008 Jul;37(7):609-17. doi: 10.1007/s00256-008-0504-x. Epub 2008 May 8. PMID: 18463865; PMCID: PMC2424184.
Sowers MF, Hayes C, Jamadar D, Capul D, Lachance L, Jannausch M, Welch G. Magnetic resonance-detected subchondral bone marrow and cartilage defect characteristics associated with pain and X-ray-defined knee osteoarthritis. Osteoarthritis Cartilage. 2003 Jun;11(6):387-93. doi: 10.1016/s1063-4584(03)00080-3. PMID: 12801478.
Zanetti M, Bruder E, Romero J, Hodler J. Bone marrow edema pattern in osteoarthritic knees: correlation between MR imaging and histologic findings. Radiology. 2000 Jun;215(3):835-40. doi:10.1148/radiology.215.3.r00jn05835. PMID: 10831707.
Ultrasound-guided tendon scraping is an emerging minimally invasive treatment for patellar tendinitis (jumper’s knee). A recent study shows promising results with faster return to sport and significant pain relief,
Read MorePatellar tendinitis (“jumper’s knee”) is a common cause of knee pain in athletes. Learn what causes it, why it lingers, and how advanced treatments like ultrasound-guided tendon scraping may help you recover faster and
Read More