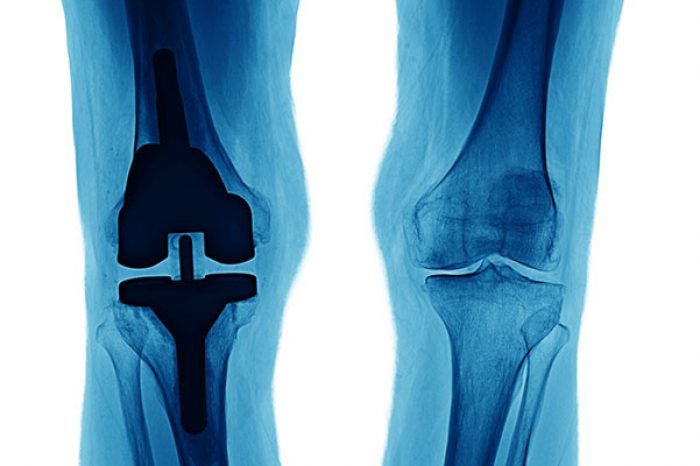

Knee osteoarthritis (OA) is one of the most common causes of pain and disability in older adults, learn more here. For many patients, total knee arthroplasty (TKA) is considered the definitive treatment once symptoms become severe. But what if there were a way to delay—or even avoid—knee replacement in select patients?
A landmark long-term study by Hernigou et al., published in International Orthopaedics, explored exactly that question. The study followed patients for an average of 15 years after receiving a subchondral bone marrow concentrate (BMC) injection in one knee, while undergoing a knee replacement on the other side
during the same surgery.
The results provide some of the most compelling long-term data we have on stem cell therapy for knee osteoarthritis.
This was not a small pilot study. It included 140 patients, aged 65 to 90, who had bilateral medial knee osteoarthritis and were already planning staged knee replacements.
Instead of replacing both knees:
One knee underwent standard total knee arthroplasty (TKA)
The contralateral knee received a subchondral injection of bone marrow concentrate (BMC) containing mesenchymal stem cells (MSCs), learn more about BMC here.
Both procedures were performed at the same time.
This design created an elegant internal control: Each patient essentially compared their own replaced knee to their stem-cell-treated knee over 15–20 years.
The rationale behind subchondral injection is critical. Learn more about intra-osseous injections here.
The authors note that:
Cartilage has no nerve supply (Dieppe & Lohmander, 2005).
Pain in osteoarthritis may originate from the highly innervated subchondral bone (Dieppe & Lohmander, 2005; Zhu et al, 2019;).
Functional fibrocartilage formation requires involvement of subchondral bone marrow (de Vries-van Melle et al, 2014; Chen et al, 2011; Lyu et al, 2021).
Mesenchymal stem cells adhere to bone and may remain locally, avoiding washout seen with intra-articular injections (Shim et al, 2015; Satué et al, 2019).
In the Hernigou et al. study:
20 mL of BMC was injected (10 mL tibia, 10 mL femur)
Concentration averaged ~7800 MSCs per mL
The hypothesis was that stimulating the subchondral marrow might:
Promote fibrocartilage production
Reduce bone marrow lesions (BMLs)
Decrease pain
Potentially delay TKA
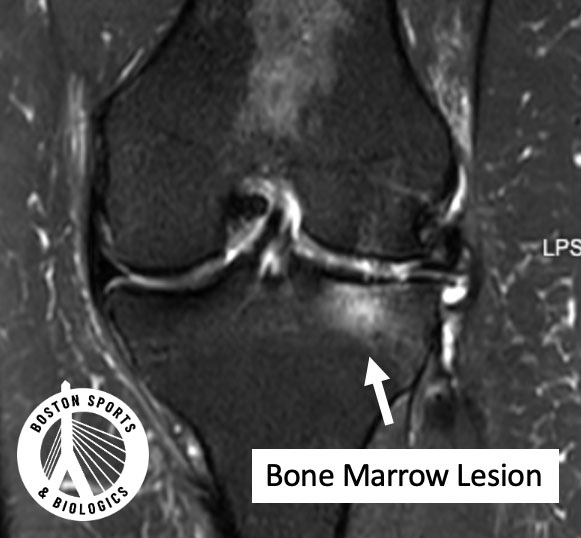
Bone marrow lesions (BMLs) are areas of abnormal signal seen on MRI. Learn more about bone marrow lesions here.
Bone marrow lesions represent:
Microfractures
Increased vascularity
Edema-like changes
Abnormal bone remodeling
Importantly:
Larger BMLs correlated with greater pain (p = 0.01)
BML size did not correlate with the severity of osteoarthritis on radiographs/x-rays
This means MRI bone findings may be more predictive than plain radiographs.
In the Hernigou et al. study, after subchondral MSC injection:
BML volume regressed over 24 months
Mean regression: ~2.1 cm³
Residual BML volume averaged 1.3 cm³
Higher numbers of progenitor cells were associated with greater BML reduction (p = 0.04)
Smaller lesions responded better than larger ones.
This suggests:
Dose matters
Lesion size matters
There may be a ceiling effect in structural reversibility
At the 15-year follow-up in the Hernigou et al. study:
115 of 140 knees (82%) avoided at total knee replacement after the bone marrow stem cell treatment.
Interestingly, this was similar to the revision rate of the replaced knees (1.00% per person-year; p = 0.34).
In other words:
The knee treated with bone marrow stem cells had a risk of future surgery comparable to revision rates of replaced knees.
More than half of patients (74 of 140) preferred their stem-cell-treated knee over the replaced knee at long-term follow-up.
Pain improvement was similar at 3 months and remained comparable at long-term follow-up.
This study does not suggest stem cell injections replace knee arthroplasty.
Instead, it suggests:
Subchondral BMC stem cell injections may meaningfully delay TKA in selected patients.
MRI-based BML evaluation is crucial for patient selection.
Perhaps most importantly:
MRI bone marrow lesions may be a stronger prognostic tool than X-rays alone.
For appropriately selected patients with knee osteoarthritis—particularly those with moderate disease and smaller bone marrow lesions—subchondral MSC therapy may offer a meaningful delay of joint replacement.
The key is patient selection, alignment correction when needed, and careful MRI evaluation.
To learn more if you are a candidate for intra-osseous bone marrow concentrate "stem cell" injections contact Boston Sports & Biologics.
In the studies referenced, bone marrow aspirate concentrate (BMAC) was shown to help delay knee replacement in some patients.
BMAC injections work by:
Rather than “regrowing cartilage,” the primary benefit is improving the biologic environment of the knee, which can lead to less pain and better function.
Ideal candidates for BMAC procedures include patients who:
Patients with advanced arthritis can still benefit, but results may be more variable.
In some cases, yes. Many patients experience meaningful symptom relief, but some may still require knee replacement in the future
PRP is often used for earlier-stage arthritis, while BMAC procedures may be considered for more advanced cases or when PRP is insufficient.
Intraosseous injection targets the bone beneath the cartilage (subchondral bone), which plays a major role in arthritis pain. This approach:
This is an advanced technique offered at Boston Sports & Biologics and other specialized centers.
Currently, BMAC and PRP injections for knee arthritis are:
However, many patients choose this option to potentially delay or avoid surgery.
Specialized centers like Boston Sports & Biologics focus on:
Choosing an experienced provider is critical for optimizing outcomes.
Chen H, Chevrier A, Hoemann CD, Sun J, Ouyang W, Buschmann MD. Characterization of subchondral bone repair for marrow-stimulated chondral defects and its relationship to articular cartilage resurfacing. Am J Sports Med. 2011 Aug;39(8):1731-40. doi: 10.1177/0363546511403282. Epub 2011 May 31. PMID: 21628638.
de Vries-van Melle ML, Narcisi R, Kops N, Koevoet WJ, Bos PK, Murphy JM, Verhaar JA, van der Kraan PM, van Osch GJ. Chondrogenesis of mesenchymal stem cells in an osteochondral environment is mediated by the subchondral bone. Tissue Eng Part A. 2014 Jan;20(1-2):23-33. doi: 10.1089/ten.TEA.2013.0080. Epub 2013 Oct 2. PMID: 23980750; PMCID: PMC3875203.
Dieppe PA, Lohmander LS. Pathogenesis and management of pain in osteoarthritis. Lancet. 2005 Mar 12-18;365(9463):965-73. doi:10.1016/S0140-6736(05)71086-2. PMID: 15766999.
Hernigou P, Delambre J, Quiennec S, Poignard A. Human bone marrow mesenchymal stem cell injection in subchondral lesions of knee osteoarthritis: a prospective randomized study versus contralateral arthroplasty at a mean fifteen year follow-up. Int Orthop. 2021 Feb;45(2):365-373. doi: 10.1007/s00264-020-04571-4. Epub 2020 Apr 23. PMID: 32322943.
Lyu J, Zhang Y, Zhu W, Li D, Lin W, Chen K, Xia J. Correlation between the subchondral bone marrow lesions and cartilage repair tissue after matrix-associated autologous chondrocyte implantation in the knee: a cross-sectional study. Acta Radiol. 2021 Aug;62(8):1072-1079. doi:10.1177/0284185120969955. Epub 2020 Nov 12. PMID: 33183061.
Satué M, Schüler C, Ginner N, Erben RG. Intra-articularly injected mesenchymal stem cells promote cartilage regeneration, but do not permanently engraft in distant organs. Sci Rep. 2019 Jul 12;9(1):10153. doi: 10.1038/s41598-019-46554-5. PMID: 31300685; PMCID: PMC6626061.
Shim G, Lee S, Han J, Kim G, Jin H, Miao W, Yi TG, Cho YK, Song SU, Oh YK. Pharmacokinetics and in vivo fate of intra-articularly transplanted human bone marrow-derived clonal mesenchymal stem cells. Stem Cells Dev. 2015 May 1;24(9):1124-32. doi: 10.1089/scd.2014.0240. Epub 2015 Jan 21. PMID: 25519508.
Zhu S, Zhu J, Zhen G, Hu Y, An S, Li Y, Zheng Q, Chen Z, Yang Y, Wan M, Skolasky RL, Cao Y, Wu T, Gao B, Yang M, Gao M, Kuliwaba J, Ni S, Wang L, Wu C, Findlay D, Eltzschig HK, Ouyang HW, Crane J, Zhou FQ, Guan Y, Dong X, Cao X. Subchondral bone osteoclasts induce sensory innervation and osteoarthritis pain. J Clin Invest. 2019 Mar 1;129(3):1076-1093. doi: 10.1172/JCI121561. Epub 2019 Feb 4. PMID: 30530994; PMCID: PMC6391093.
Ultrasound-guided tendon scraping is an emerging minimally invasive treatment for patellar tendinitis (jumper’s knee). A recent study shows promising results with faster return to sport and significant pain relief,
Read MorePatellar tendinitis (“jumper’s knee”) is a common cause of knee pain in athletes. Learn what causes it, why it lingers, and how advanced treatments like ultrasound-guided tendon scraping may help you recover faster and
Read More